

By Anne Klockenkemper, Anna Capizzi, and Matthew Palmer
CatholicU, Fall 2023
As Elizabeth Mastoros, B.S.N. 2023, neared graduation this past spring, she was able to glimpse the future of education on campus for Conway School of Nursing students. It floored her.
Mastoros, a former Conway Scholar who is now a labor and delivery nurse at Holy Cross Hospital in Silver Spring, Md., took part in a series of demonstrations of new simulation technologies that will be used once the nursing building, now under construction, opens in 2024.
Before they even set foot in a physical hospital, students will gain experience walking down the halls of hospitals or performing procedures — all in the metaverse.
The new technology will include a virtual hospital — a 3D-screen-based environment that will be accessed via a computer to help students strengthen critical thinking skills — and virtual reality headsets for practicing clinical procedural skills.
These technological innovations, happening right in the heart of the University’s campus, will be a central part of the Conway School of Nursing’s program.
“New simulations can help expose both students and nurses alike to different clinical scenarios and better prepare us for real-world situations,” Mastoros said. “Part of nursing is a commitment to lifelong learning. I think incorporating this new (simulation) technology definitely contributes to that.”
According to David Want, M.S.N. 2017, D.N.P. 2020, who is chair of the nursing school’s Simulation Committee and assistant clinical professor, the University has found a way for the metaverse to thrive within its mission of excellence in teaching.
“It is the art of the possible, involving the innovative use of immersive technologies such as extended reality — augmented and virtual reality — and other technology-enabled simulation-based and experiential learning modalities to create a virtual world with which we interact either on a computer screen or through augmented or virtual reality headsets or glasses,” said Want.
This new technology will build upon immersive learning already in use at the Tersigni Simulation Center in Gowan Hall to simulate experiences students may encounter in real-world practice.

The new 102,000 square-foot, $84 million nursing and sciences building under construction along Michigan Avenue will include the new Cesar A. Caceres Simulation Center that will provide four times the space that exists in Tersigni. Funded through a gift from the Institute for Technology in Health Care, the center will include multiple spaces, such as high fidelity patient rooms that provide an acute care experience, a recovery room, and a debriefing room where student performance during simulations can be reviewed.
All undergraduate nursing students, about 150 to 200 per week, use the current simulation center. Want said the number will increase to 375 to 450 students per week when the Caceres Center is in use in the new building. What they learn is applied to clinical scenarios that include conducting a health assessment or a physical exam, as well as working on their therapeutic communication skills.
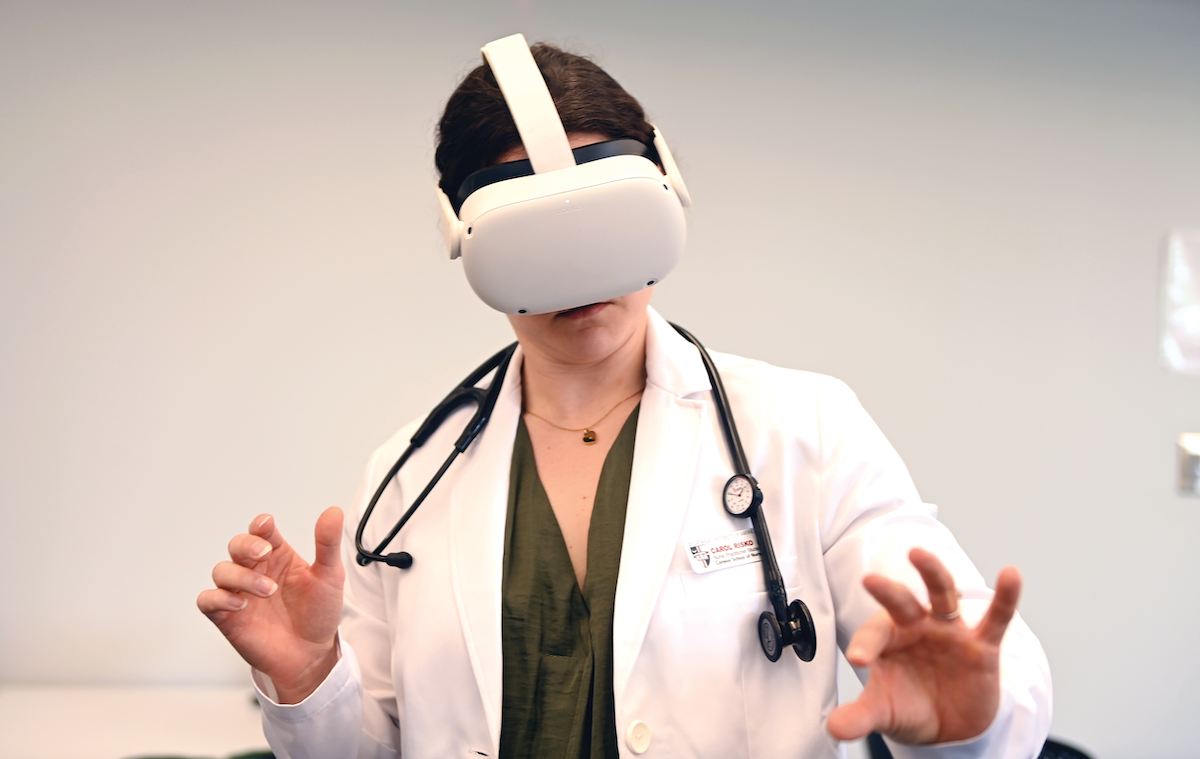
In the building’s virtual reality suite, students will wear VR goggles or may work in an augmented reality setting with scenes projected onto the walls.
“I have never used VR before but was able to navigate it with ease as there were built-in instructions to guide users through,” Mastoros said. “We were also able to give real-time feedback to the developers to help make the programs the best possible for our Conway School of Nursing curriculum."
Tata Consultancy Services is developing the VR headset technology that will be implemented in the new nursing building, along with another innovative educational product, the virtual hospital.
This 3D technology, seen on a 2D screen, will help undergraduate nursing students “practice prioritizing patients. It might be expanded in the future for graduate students,” said Jeanne Moore, associate dean for innovation and online learning, clinical associate professor, director of the family nurse practitioner program, and a member of the simulation committee.
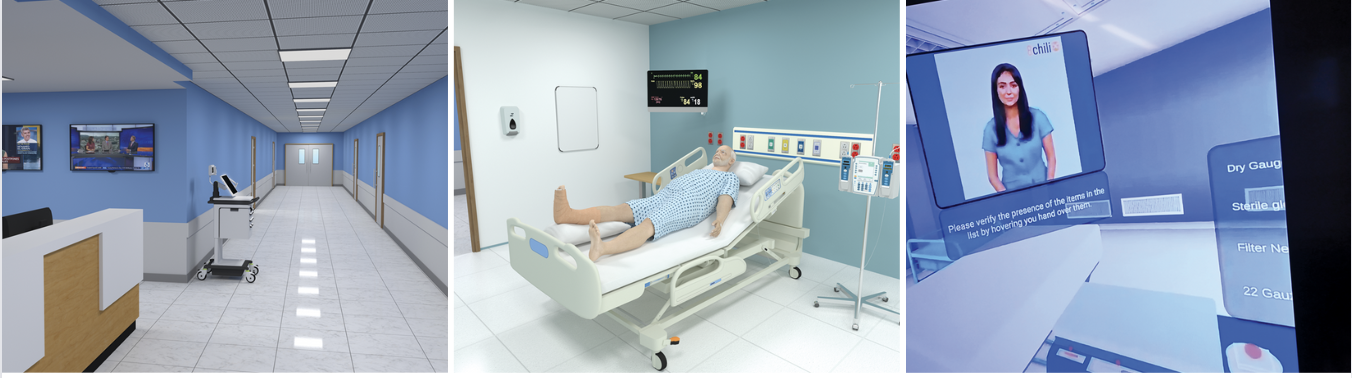
The virtual hospital “is an on-screen experience of virtually walking down the hall in a hospital and going into the rooms of different patients, reading their electronic patient record, assessing the patient, and making decisions about care,” said Conway School of Nursing Dean Marie Nolan, Ph.D. 1989.
The hope is that this virtual hospital will eventually include multiple wings, including an emergency room, pediatric care, and an intensive care unit.
To make a situation more true to life, interruptions will be programmed into the experience. That way, Nolan said, with the needs of other patients built in, a student will learn to make decisions regarding whether to turn to the needs of another patient or to delegate aspects of care to a patient care tech and continue caring for the current patient. This will allow students to practice making decisions about prioritizing multiple aspects of care for multiple patients at the same time.
“Chief nursing officers from among our clinical partner hospitals have mentioned that it is common among new nursing graduates from all schools of nursing to initially find caring for multiple patients with competing priorities to be a challenge,” Nolan said.
While students will naturally become more comfortable over time and with practice, she said faculty wanted to figure out a way to provide additional experiences that will help them prepare to decide the best way to triage the needs of multiple people.
Want said that the COVID-19 pandemic magnified the need for simulation-based learning that involves technology such as virtual or augmented reality.
“Simulation is essentially built off experiential learning theory. It provides a safe space to practice and learn and make mistakes without the risk of harming a patient. Students then transfer those skills to real-life patients,” he said. “It’s a tool that produces better nurses that results in better outcomes and healthier people.”
Nolan said the VR goggle technology will provide a different experience by enabling students to practice procedures. One simulated procedure that has already been tested is the lumbar puncture.
“Pediatric nurse practitioners must learn to perform lumbar punctures on infants to test spinal fluid for signs of an infection,” she said. “The student ‘sees’ the lumbar puncture tray on the table and virtually picks up and opens sterile wipes, a drape, a needle, collection tubules, and a bandage and uses these items to perform the procedure on a virtual infant.”
Because the procedure is incredibly complicated — there are more than 50 separate steps — this virtual simulation will allow the students to practice them all; first in a novice mode that offers them prompts on taking the next step in the procedure, and then later in an assessment mode that simulates the procedure without the prompts and provides a score.
Zachary Brotzman, B.S.N. 2023, a former Conway Scholar who currently is a nurse with the pediatric cardiac intensive care unit at Johns Hopkins Children’s Center in Baltimore, was one of the students who tested the technology planned for the new building.
“I was really, really excited to see how realistic it was and how interactive the environment was. That technology was really quite intuitive,” he said. At the time, “I was going into pediatrics and it was really quite exciting to see a pediatric patient being able to be interacted with in the virtual reality setting.”
It gave him “more awareness of what the world of pediatrics looks like,” Brotzman added.
The lumbar puncture VR procedure was designed for graduate nurse practitioner students, mainly acute care pediatric nurse practitioners. But, according to Moore, the procedure could be expanded to adult patients in the future.
“Allowing nurse practitioner students to practice it multiple times before being tested for competency — and before performing it on an actual infant — is a major contribution to nursing education and quality patient care,” Nolan added.
With both of these products, students will be better acclimated to some of the real-world situations they might face.
The simulations are still being refined. For example, Nolan said some faculty thought that the lumbar puncture simulation should include the sound of the baby crying since this sometimes occurs in the actual procedure.
“These immersive technology simulations are examples of some of the many approaches that our faculty use in the simulation center to prepare students to deliver high quality and compassionate care that respects the dignity of the human person,” Nolan said.
Mastoros, once a virtual reality neophyte, is already using the tools learned in the metaverse, including virtual reality sessions, to help her patients. The future is here, she said.
“I hope future nursing students embrace the technology in conjunction with their physical classroom environment,” Mastoros said. “VR technology has certainly helped me to become a well-rounded nurse. As my career is just beginning, I can use the tools I learned through the VR environment to help real-life people.”